While vasectomies can seem like an extreme solution, they are actually very practical. Find out everything you need to know and see if a vasectomy is right for you.

reviews

reviews

A vasectomy is a simple operation performed on an adult male to prevent impregnation of a female partner during vaginal intercourse.
The operation stops sperm from entering the semen during ejaculation. Without sperm present, even a healthy egg cannot become fertilized in a woman's reproductive organs and the woman will not become pregnant.
Vasectomy does not affect erections, orgasm or ejaculation.
It blocks the flow of sperm which makes up only 1-2% of ejaculate volume so patients or partners won’t notice any difference. For this reason, it is sometimes referred to as "male sterilization."
Before we jump in further, let's cover the most frequently asked questions about vasectomies.
Vasectomies range in cost from $300 to $3,000, including follow-up appointments. The cost of a vasectomy depends on where it is performed, what methods are used, and how much is covered by your insurance.
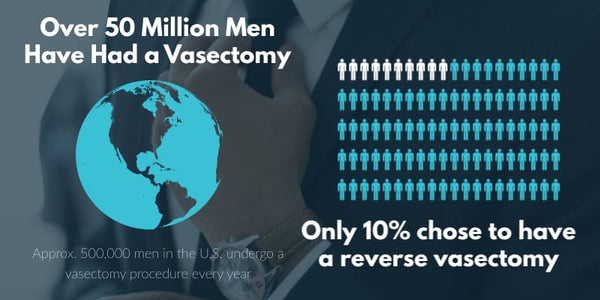
Vasectomies can be reversed but are designed to be permanent. Vasectomy reversals are less likely to be covered by insurance. Expect to fork up anywhere from $3,500 to $15,000 for full vasectomy reversal.
A vasectomy has no effect on sexual arousal, orgasm, or ejaculation. A vasectomy will neither cause premature ejaculation nor will it eliminate premature ejaculation.
No, a vasectomy affects none of your hormone levels, including testosterone. It merely prevents your testicles from supplying sperm to the seminal vesicles.
A vasectomy is performed by a doctor in his or her office or clinic. The doctor makes small cuts in the scrotum to access the vas deferens, tubes that connect the testicles to the seminal vesicles and supply sperm to the seminal mixture. 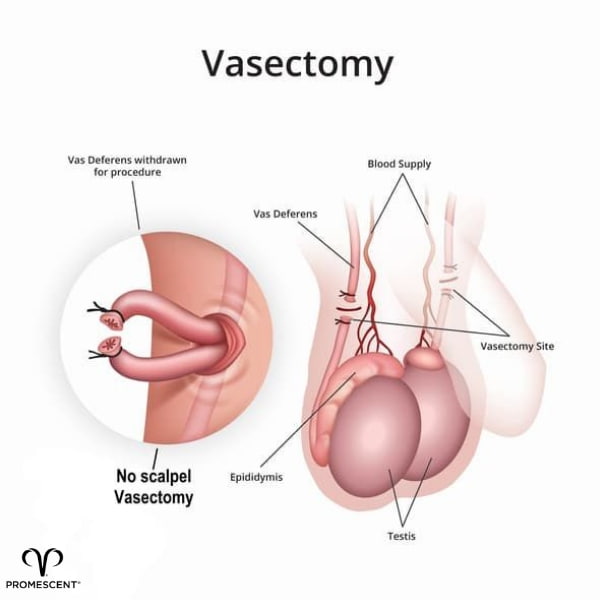
The doctor will cut the vas deferens so that semen can no longer be delivered to the seminal vesicles.
The doctor might accomplish this by:
The procedure may be accomplished with one cut, or with two. Doctors have two options for the cutting method:
The aptly-named "no-scalpel" method of vasectomy uses no scalpel for the incision.
Instead, the doctor makes a single small opening in the scrotum, spreads it open, removes a small segment of the vas deferens through the small opening, clamps it, and completes the procedure with the vas deferens outside the body.
The doctor then seals or cauterizes the cut ends of the vas deferens and replaces them in the scrotum. This procedure is usually faster than the incision method and requires no stitches.
The incision method of vasectomy involves two small cuts made with a scalpel on either side of the scrotum.
The doctor can then remove a portion of the vas deferens and seal the cut ends by tying them, sealing them, or cauterizing them with a minor electrical current. The incisions in the scrotum are then sealed with stitches.
The procedure usually takes about 10 - 20 minutes under local anesthetic or conscious sedation ("twilight anesthesia").
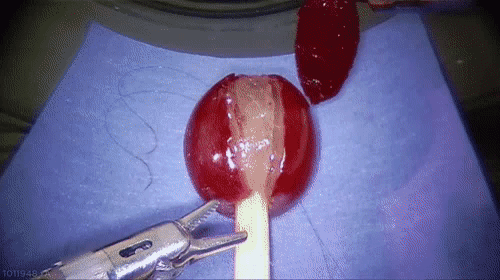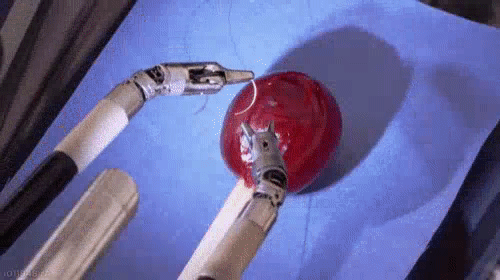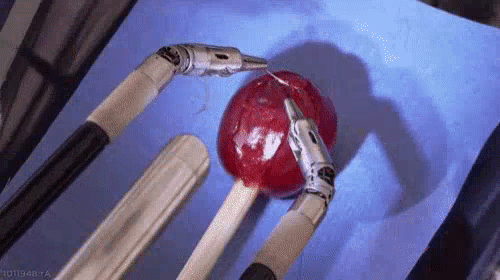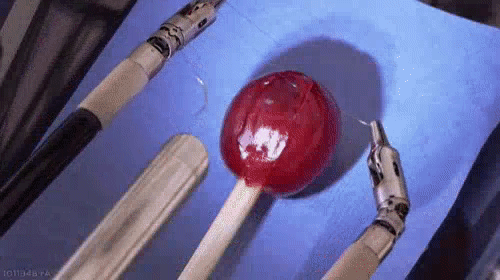
Because it is faster and requires no stitches, the no-scalpel method is becoming more common.
In addition to these benefits, no-scalpel vasectomies have shown to carry less than 5% the risk of blood clots, infection, and other complications.
Talk to your doctor about which method is best for you.
Both methods are outpatient procedures that do not require a general anesthetic.
As a method of birth control, a vasectomy is close to 100% effective. The separated or blocked vas deferens rarely reconnect on their own.
Note; sperm may still be present in the seminal vesicles up to three months or longer after the procedure.
Continue using your current method of birth control until your doctor confirms on a follow-up appointment that your semen is free of sperm.
Less than 1% of vasectomies fail.
They are designed to be a permanent, reliable procedure to sterilize the semen of an adult male.
After the vasectomy has been confirmed to be effective, a man can expect to have vaginal intercourse as often as desired, with no other form of birth control, and never fertilize the eggs of his partner.
Note; that vasectomy does not guard against sexually transmitted diseases or infections.
Vasectomies are designed to be permanent but can be reversed with a second procedure.
However, vasectomies are only recommended for men who are very confident that they no longer want to father biological children via fertilization through vaginal intercourse.
Even in that circumstance, the vasectomy does not prevent the transmission of many sexually transmitted infections, so condom use is still recommended under a variety of circumstances.
In practice, vasectomies can often be reversed through a second procedure to re-attach the vas deferens.
Be advised, that the procedure to reverse a vasectomy is much more complicated than the vasectomy itself—longer, more invasive, with a more disruptive and uncomfortable recovery process.
Vasectomy Advantages
A vasectomy is relatively safe. Complications are rare, but could include:
Vasectomies range in cost from $300 to $3,000, including follow-up appointments. The cost of a vasectomy depends on where it is performed, what methods are used, and how much is covered by insurance.
Most health insurance plans will cover some or part of an outpatient vasectomy procedure.
Note; deductibles, co-insurance, and out-of-pocket maximums may apply, so you may still owe money even if your insurance technically covers the procedure.
If you don't have health insurance, your state's Medicaid programs may cover some of the costs.
Health insurance may not cover any of the costs of reversing a vasectomy. Expect to fork up anywhere from $3,500 to $15,000 for full vasectomy reversal.
Also, keep in mind that your fertility success rate will vary greatly.
No, a vasectomy affects none of your hormone levels, including testosterone. It merely prevents your testicles from supplying sperm to the seminal vesicles.
Testosterone is supplied to the body through a different mechanism.
Reports of a vasectomy negatively affecting a man's sexual performance are rare.
In fact, studies performed in 2015 by Stanford University indicate that men who have vasectomies tend to have more sex than men who have not had vasectomies.
A study performed in 2017 by Frankfurt University found that test subjects reported increased sex drives after undergoing a vasectomy.
The vas deferens plays no role in erection, orgasm, or ejaculation. Cutting them has no effect on sexual performance other than depriving the semen of sperm.
Note that in rare cases, sperm can continue to live in the seminal vesicles up to three months after the procedure. Typically, a semen analysis will be conducted at 6 weeks and 98% of men have no sperm, however, 1-2 will have non-motile sperm.
A vasectomy has no effect on sexual arousal, orgasm, or ejaculation.
A vasectomy will neither cause premature ejaculation nor will it eliminate premature ejaculation. Men suffering from premature ejaculation must treat the condition by other means, such as a climax control spray.
A vasectomy does not affect erectile tissue, which fills with blood upon arousal and causes the penis to become erect, either through sexual activity with a partner or through masturbation.
Neither does a vasectomy affect the mechanisms of male sexual arousal. A vasectomy is highly unlikely to cause or cure any form of erectile dysfunction.
A vasectomy is the only form of medical sterilization currently available to males.
Men concerned about the procedure or its after-effects must rely on other forms of birth control to prevent pregnancy.
While condoms are inexpensive, they are disposable. Over the long run, a vasectomy may actually be cheaper than condom use.
Based on reports by the Kinsey Institute on the sexual behavior of males between the ages of 18 and 69, the average male has sex 3,804 times. Conservatively estimating a cost of $0.75 per condom, the average male in question would spend $2,853 on condoms!
Impeccable use of condoms prevents pregnancy 98% of the time. Many people fail to use condoms properly, however, resulting in an effective prevention rate of only 85%. By contrast, a vasectomy is over 99% effective.
Many people prefer the sensation of sexual intercourse without condoms, making a vasectomy an attractive option compared to condom use.
Importantly, a vasectomy has no effect on the transmission of sexually-transmitted diseases or infections, while condoms greatly reduce their spread when used properly.
Condom use is therefore recommended for sexual intercourse outside of trusted, monogamous or "fluid-bonded" relationships.
Fluid-bonded partners only use condoms with other sexual partners, using no condoms while having intercourse together.
The "pull-out method," also known as "coitus interruptus," "withdrawal," or "pull-and-pray," is one of the most ancient forms of birth control, particularly in remote or impoverished areas.
When performed perfectly, it has a success rate of 96% to 98% in preventing pregnancy.
However, sperm can still be present in pre-ejaculatory fluid emitted by the penis. The pull-out method is therefore widely considered an unreliable form of birth control, especially stacked up against the 98.85% effectiveness of vasectomy in preventing pregnancy.
Many couples prefer the sensation and intimacy of the male ejaculating inside the vagina, making a vasectomy more attractive for long-term sexual satisfaction.
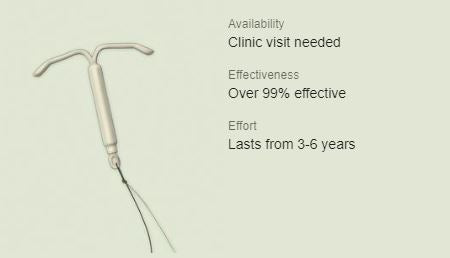
A female intrauterine device (IUD) is one of the most effective forms of reversible contraception. The device lasts up to ten years, but insertion and removal can cause the woman discomfort. Discomfort after insertion is rare.
The failure rate of an IUD has been estimated between 0.2% and 0.8%—highly effective compared to other methods, but still less effective than vasectomy with its 0.15% failure rate.
You can start having sexual activity as soon as the post-operative discomfort subsides and you feel up to it.
As discussed before, however, other methods of birth control should continue to be used until the semen is confirmed to be sperm-free in follow-up lab tests.
This could be up to three months, twenty ejaculations, or even longer after the operation. Until this time, live sperm remaining in the seminal vesicles could still impregnate a partner.
Recovering from a vasectomy may vary among patients but typically patients who undergo procedure on Friday will make it to work on Monday.
The scrotum has been cut and must heal. This process can entail some pain or mild discomfort, bruising, and/or swelling. Mild or moderate painkillers will usually ease the recovery.
Speak to your doctor if pain persists and you think you need stronger pain-management medication.
The first several ejaculations after the procedure may contain blood. This might look alarming, but is no cause for concern. The semen will abate shortly.
Dr. Jed Kaminetsky M.D. is an American Board Certified Urologist and earned his Medical Degree at New York University. In his tenure he became a member of the American Urological Association and the American College of Surgeons. Dr. Kaminetsky pioneered the minimally invasive Rezum BPH treatment and is an expert in male and female dysfunction.
Absorption Pharmaceuticals LLC (Promescent) has strict informational citing guidelines and relies on peer-reviewed studies, academic or research institutions, medical associations, and medical experts. We attempt to use primary sources and refrain from using tertiary references and only citing trustworthy sources. Each article is reviewed, written, and updated by Medical Professionals or authoritative Experts in a specific, related field of practice. You can find out more about how we ensure our content is accurate and current by reading our editorial policy.
Mayo Clinic Staff. 2021, August 21. Vasectomy. The Mayo Clinic. https://www.mayoclinic.org/tests-procedures/vasectomy/about/pac-20384580#:~:text=Vasectomy%20is%20a%20form%20of,outpatient%20setting%20under%20local%20anesthesia.
National Institute of Health. 2016, December 1. How is a vasectomy done?. US Department of Health and Human Services. https://www.nichd.nih.gov/health/topics/vasectomy/conditioninfo/done#:~:text=With%20the%20%22no%2Dscalpel%22,then%20put%20back%20in%20place.
S Q Li, M Goldstein, J Zhu, D Huber. 1991 Feb. Vasectomy Techniques. National Library of Medicine. https://pubmed.ncbi.nlm.nih.gov/1988727/
American Family Physician Staff. 1999 July 1. American Family Physician. https://www.aafp.org/afp/1999/0701/p137.html
National Institute of Health Staff. 2016, December 1. How effective is vasectomy?. US Department of Health and Human Services. https://www.nichd.nih.gov/health/topics/vasectomy/conditioninfo/effective
Mayo Clinic Staff. 2021, August 20. Vasectomy reversal. The Mayo Clinic. https://www.mayoclinic.org/tests-procedures/vasectomy-reversal/about/pac-20384537?ref=3827979.b0876e
National Institute of Health Staff. 2021, December 1. What are the risks of vasectomy? US Department of Health and Human Services. https://www.nichd.nih.gov/health/topics/vasectomy/conditioninfo/risk
Dawn Stacey, PhD, LMHC. 2022 January 12. The Cost of a Vasectomy. Verywell Health. https://www.verywellhealth.com/how-much-does-a-vasectomy-cost-906900
Louise Norris. 2021 March 20. How to Choose the Best Health Insurance Plan for You. Verywell Health. https://www.verywellhealth.com/health-insurance-4014713
Regan Olsson. 2019, December 13. Why He Doesn’t Want a Vasectomy (And What You Can Do About It). Banner Health. https://www.bannerhealth.com/healthcareblog/teach-me/five-vasectomy-myths-debunked#:~:text=A%20vasectomy%20interrupts%20the%20flow,change%20testosterone%20level%20or%20libido.
Cent European Journal of Urology Staff. 2017 June 23. Impact of vasectomy on the sexual satisfaction of couples: experience from a specialized clinic. National Library of Medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5656365/#
Times Now Digital Staff. 2017, November 21. Men have higher sex drive after having a vasectomy. Times Now News. https://www.timesnownews.com/health/article/men-have-higher-sex-drive-after-having-a-vasectomy/130117?ref=3827979.b0876e
Marie Stopes Staff. 2020, November 23. Vasectomy vs Condoms: the real cost of condoms. Marie Stopes Australia. https://www.vasectomy.org.au/faqs/condoms-vs-vasectomy/?ref=3827979.b0876e
Planned Parenthood Staff. (n.d). How effective are condoms? Planned Parenthood. https://www.plannedparenthood.org/learn/birth-control/condom/how-effective-are-condoms?ref=3827979.b0876e
Traci C. Johnson, MD. 2021, May 06. Birth Control and the IUD (Intrauterine Device). WebMD. https://www.webmd.com/sex/birth-control/iud-intrauterine-device?ref=3827979.b0876e#1
Alana Biggers, M.D., MPH. 2018, January 22. Everything you need to know about vasectomy. Medical News Today. https://www.medicalnewstoday.com/articles/265127

reviews
Your Cart Is Empty